Search
Showing results for "Childhood interstitial lung disease "
Antimicrobial resistance is a current global health crisis, and the increasing emergence of multidrug resistant infections has led to the resurgent interest in bacteriophages as an alternative treatment.

In an exciting development for the Wal-yan Respiratory Research Centre, Professor André Schultz has been appointed as the Centre’s new Head, succeeding Professor Stephen Stick.
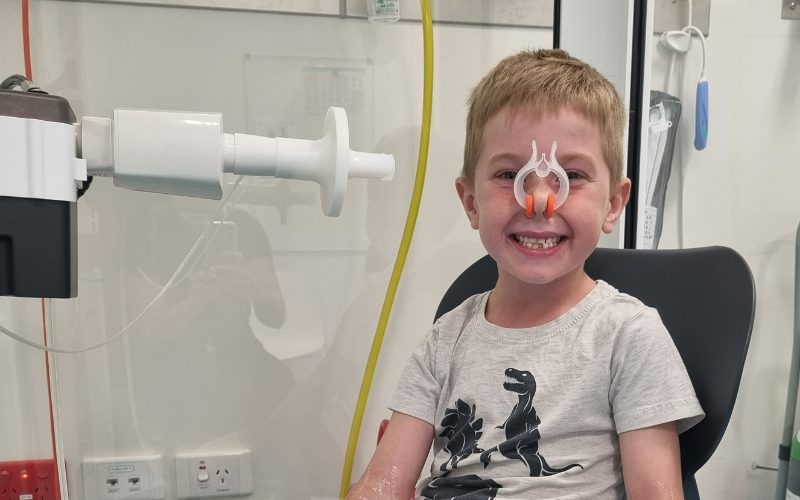
A new study to determine if it’s safe for children who were born preterm to attend day care officially commenced this month.
There is no published information on preterm children's activities and participation during middle childhood, a time when growth and development are characterised by increasing motor, reasoning, self-regulation, social and executive functioning skills. This study explored the health, activities and participation of children born very preterm during middle childhood (6-9 years) from the perspectives of their parents.
This review focuses on the scientific rationale for early intervention aimed at asthma prophylaxis and discusses therapeutic approaches

Preterm researchers Dr Shannon Simpson (left) and Professor Jane Pillow (right) with Tony Sparks WA chairperson Amber Bates.
The Airway Epithelial Research Team is investigating the role of the epithelium in the development of airway diseases including asthma, cystic fibrosis and lung transplant rejection.
When babies are born early or ‘preterm’ their tiny bodies are put under a lot of stress that can result in health problems in later life.
Nasal epithelial cells from very preterm infants have a functional defect in their ability to repair beyond the first year of life, and failed repair may be associated with antenatal steroid exposure.
In children, chronic wet cough may be a sign of underlying lung disease, including protracted bacterial bronchitis (PBB) and bronchiectasis. Chronic (> 4 weeks in duration) wet cough (without indicators pointing to alternative causes) that responds to antibiotic treatment is diagnostic of PBB. Timely recognition and management of PBB can prevent disease progression to irreversible bronchiectasis with lifelong consequences. However, detection and management require timely health-seeking by carers and effective management by clinicians.
